We suggested a reoperation but the patient declined. The ILM flap was not covering the MH but remained attached where it had not been peeled ( Fig. However, the MH was noted in the OCT images to be open at two weeks after the surgery. The coverage of the MH by the ILM flap was confirmed on postoperative day 3 by optical coherence tomography (OCT Fig. The patient was instructed to maintain face-down positioning for three days. Then the ILM was folded over but not pushed into the MH, and fluid-gas exchange was performed to tamponade the flap against the retina. The flap was hinged at the superior border of the macular hole. 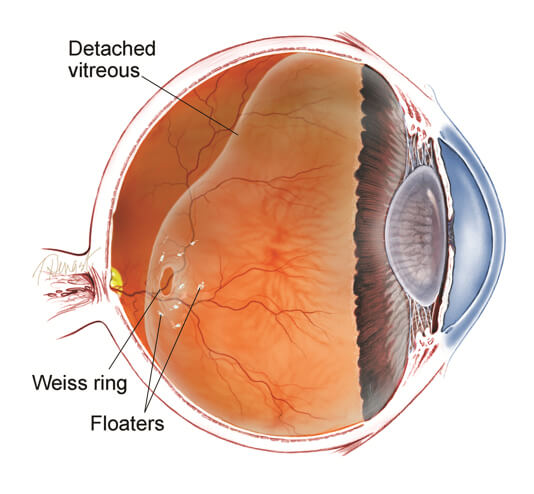
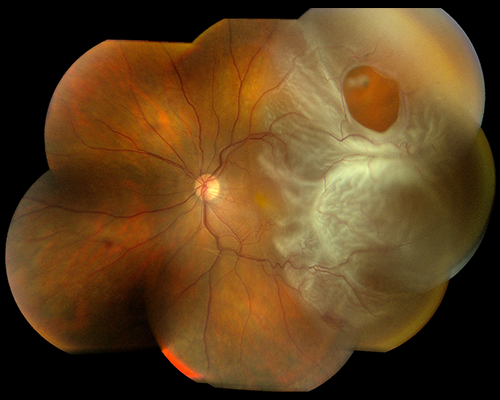
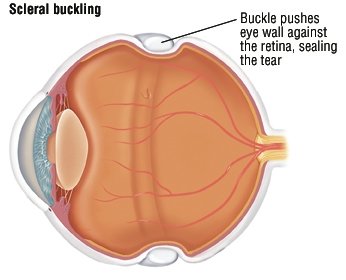
Brilliant blue G (ILM blue, DORC, Netherland) was used to make the ILM more visible, and the superior half of the ILM adjacent to the MH was peeled off the retina. She underwent pars plana vitrectomy (PPV) combined with phacoemulsification and implantation of an intraocular lens with a 25-gauge system by one of the authors (TB). Optical coherence tomography (OCT) revealed a full-thickness macular hole with a diameter of 630 μm (b). It is important for persons with significant nearsightedness or with family histories of retinal detachments to have periodic eye examinations so that changes in the vitreous or retina may be diagnosed and potential retinal detachments prevented.Preoperative photograph and optical coherence tomographic image of a macular hole.Ī stage 3 macular hole can be seen in the left eye of a 70-year-old Japanese woman. Patients with symptoms of retinal detachments require prompt attention by an ophthalmologist. Occasionally, more than one operation may be required. Over 90% of all retinal detachments can be reattached by modern surgical techniques. Should a detachment be present, surgical treatment becomes necessary to save sight in the eye. The same results can be accomplished by freezing the back wall of the eye behind the retinal tear. This produces scars that seal down the edges of the tear and prevent fluid from passing through. If the retina is torn and not yet detached, a laser may be used to place small burns around the edge of the tear. The part of the retina that is detached will not work properly and you will notice a blur or a blind spot. Once a retinal tear is present, watery fluid from the eye may pass through the hole and cause separation from the retina and the back of the eye. 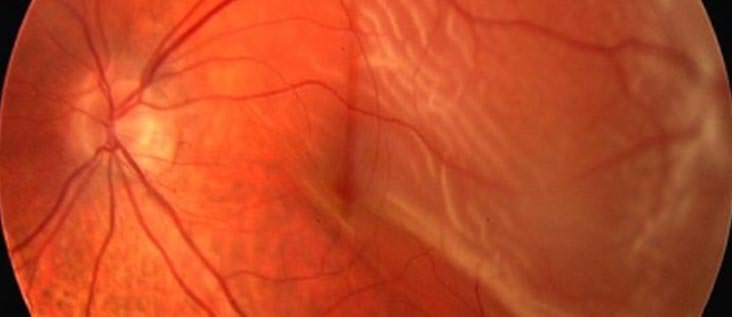
Normal aging can sometimes cause the retina to thin and deteriorate, but more often shrinkage of the clear gel-like substance which fills the center of the eye is responsible for deterioration and retinal tears. Small tears or holes in the retina cause most retinal detachments. If the detachment occurs suddenly, a patient may experience a total loss of vision in one eye. Further development of a detachment will blur central vision and create significant sight loss in one eye. Symptoms of a retinal detachment include noticeable floaters or light flashes, wavy or water lines in their overall vision or the appearance of a dark shadow in some part of their side vision. If not treated early, a retinal detachment may lead to permanent loss of vision. A hard blow to the eye can cause a detachment as well. A retinal detachment is more likely to develop in people who are nearsighted or those with relatives who have had a detachment. It is a serious eye problem that may occur at any age although usually in middle-aged or older individuals. A retinal detachment will effect one out of every 10,000 people each year in the United States. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
